Anatomy
The hip is a ball-and-socket joint located at the pelvis, with the acetabulum making the “socket” side of the joint, and the head of the femur, making up the “ball” side of the joint.
Both sides of the joint are covered in hyaline cartilage, the same as other joints within our body. This gives the joint the ability to glide smoothly through its ranges of motion. Underneath the cartilage lies subchondral bone, which is harder in consistency than areas found at the middle, or metaphysis, of bone.
Osteoarthritis (OA) of the hip is the wearing down, and possibly erosion of the cartilage surfaces within the hip joint. This may be caused by several factors.
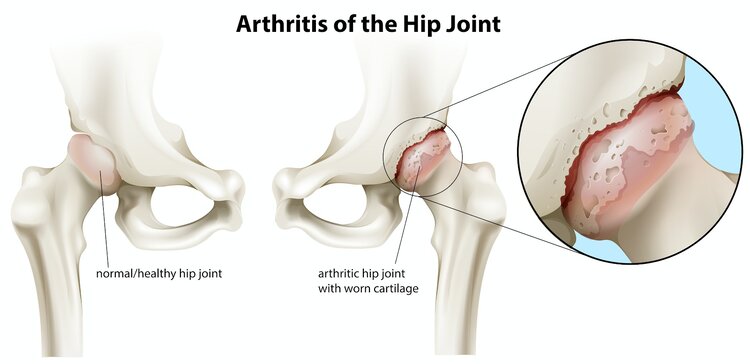
Osteoarthritis of the hip
Etiology
Hip osteoarthritis is thought to originate due to multiple risk factors:
-
Abnormal hip morphology, or shape:
-
Presence of hip dysplasia (See hip dysplasia info page for more information)
-
Femoroacetabular Impingement or FAI (see FAI page for more information)
-
Abnormal alignment of the femur
-
-
Mechanical Injury to cartilage (impact from fall or accident)
-
Hip muscle weakness
-
Underlying systemic disease
-
Advanced Age
-
Ethnicity
-
Genetics – There is a 60% risk of developing OA from genetic factors if there is a prior history of hip OA within the same family.
-
Obesity – For every 5 unit increase in BMI (body mass index), there is an 11% increase in risk for developing hip OA.
Hip osteoarthritis affects approximately 25% of those surviving to 85 years of age, with a lifetime risk of requiring a total hip arthroplasty of 10%. That means 1 in 10 people will need a major surgery to address their advanced hip arthritis!
Diagnosis
Hip OA is mainly a radiographic diagnosis, meaning that it is diagnosed based off of parameters and measurements found on plain x-rays of the pelvis and hips.
Hip osteoarthritis is graded on a scale of 0 to 4:

Treatment
Hip Osteoarthritis treatment generally progresses in stages, depending on the cause and stage of the disease. It is worth noting that once the osteoarthritis process has begun, the aim in treatment is to slow the progression of the disease and manage the symptoms effectively while preserving adequate function. Therefore, treatment begins with prevention of the disease or limiting the progression of the disease.
Modifiable Risk Factors That Help To Decrease The Chance For Hip Arthritis Include:
-
Weight loss
-
Routine aerobic exercise and strengthening
-
Treatment of underlying abnormal hip morphology (i.e. hip impingement, dysplasia, abnormal femoral torsion or rotation)
Conservative Care Options:
-
Weight loss – Having a body weight as close as possible to ideal (BMI of 25) can decrease the amount of joint reactive force through the hip by a multiple of 3. For example, for every 5 pounds overweight you are above the hip joint, 15 pounds of force are placed through the hip joint during weight bearing positions.
-
Physical therapy – strengthening of the hip and core musculature may relieve excess force through the hip joint, decreasing inflammation and therefore pain within the arthritic hip.
-
Oral medications – Non-steroidal anti-inflammatory (NSAIDs) medications are typically the safest medications to use when no other health conditions exist. In some cases, these medications may not be utilized.
-
Activity modifications – avoidance of pain-inducing positions like hip flexion, or high impact activities like jogging or jumping.
-
Injections:
-
Steroid injections may offer temporary relief of pain in an effort to improve conditioning of the hip’s supporting musculature and soft tissues.
-
Biologic injections – Stem cell (BMAC) or PRP injections have shown promising results with pain reduction and functional improvements in mild to moderate osteoarthritis of the hip for up to two years per injection series
-
There are currently exciting new non-surgical treatments for osteoarthritis under investigation that aim to slow arthritis progression, and possibly even re-grow cartilage. Although these investigations are in early stages, there is hope that in the near to mid-term future for newer, more effective conservative management options to treat osteoarthritis.
Surgical Care Options:
-
Total hip arthroplasty – Total hip arthroplasty is the gold standard procedure for end stage osteoarthritis of the hip. Over 1.2 million total hip arthroplasties, or hip replacements, are performed each year worldwide.
Dr. Andrew Dold, MD specializes in both hip arthroscopy and hip arthroplasty procedures. For a consultation with Dr. Dold, please enter your information HERE and a member of our team will contact you within 24 hours.


