Definition:
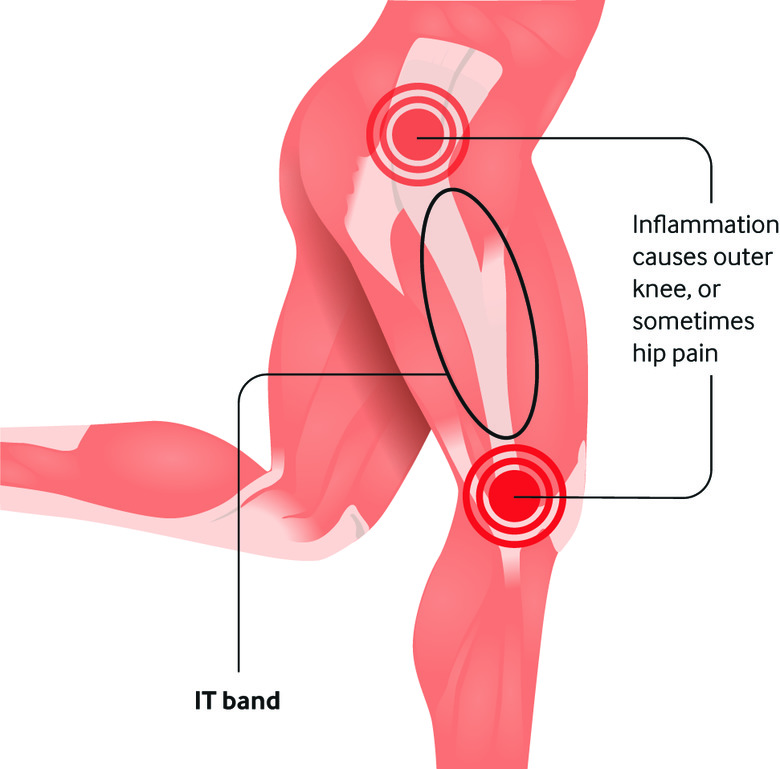
The iliotibial band or IT band is a tendon that begins at the iliac crest and distally inserts at Gerdy’s tubercle which is located on the anterolateral surface of the proximal tibia. The IT band is a continuation of the tensor fascia lata. Moreover, the IT band runs from the top of your pelvis to the lateral aspect of the knee (Think: Iliac Crest to Tibia is “IT band”). IT band syndrome occurs when this tendon creates increased friction with the lateral femoral condyle. This friction can cause inflammation and pain on the outside of the knee, which is more common in patient performing repetitive flexion-extension exercises of the knee (ex. Runners). Occasionally, the pain will extend into the side of the thigh and hip. Lateral knee pain is usually present during activity and is improved with rest. IT band syndrome can be present bilaterally (both legs) and usually comes on after a short period of exercise (running) while that condition is active.
Etiology:
IT band syndrome is caused by repetitive extension and flexion of the knee leading to the IT band shifting forward and backward along the lateral femoral condyle. This is commonly caused by tightness and imbalance of the tensor fascia lata, proximally. It is common in distance runners and endurance cyclists. IT band syndrome is classically an overuse injury. It is often seen in those quickly increasing their mileage or activity level. Again, the problem originates at the hip (due to the tensor fascia lata), but causes symptoms at the knee (lateral-sided knee pain). Therapy should be directed at the hip to correct the tightness of the IT band caused by the tensor fascia lata.
Factors that may increase your risk of IT band syndrome include:
- Weak hip abductors
- Weakness of the quadriceps or hamstring muscles
- Excessive foot pronation
- Tightness of the IT band or Tensor Fascia Lata
Diagnosis:
IT band syndrome is generally diagnosed clinically with a thorough history and physical exam by your provider. Advanced imaging (MRI) is typically not required.
History:
Patients often present with pain on the lateral side of the knee. Pain may also occur in the hip and thigh. Symptoms often occurs after patients increase their activity or runners up their mileage. It can also occur in the post operative setting for patients who have undergone a total hip or knee arthroplasty, where the alignment of their lower extremity has changed due to surgery. Pain is often an aching or burning sensation which increases with activity. Runners will typically report that the pain begins shortly after they start running, and decreases when they stop or rest for a period of time. However, when they resume running, the pain recurs along the lateral side of the knee. The pain is sharp and forces them to run with a limp.
Physical Exam:
During physical examination, there is often localized tenderness over the outside of the knee at the lateral femoral condyle. There may be clicking or popping associated with knee range of motion. Decreased range of motion of the hip or knee can be found as well as weakness of hip abduction. A positive Ober’s test helps to determine the diagnosis of IT Band syndrome. Your provider may ask you to perform a single leg squat and, in the setting of IT band syndrome, this might exacerbate the lateral-sided knee pain.
Imaging:
Advanced imaging, such as an MRI, is typically not required to make the diagnosis of IT band syndrome. X-rays are recommended for all patients presenting with knee pain. X-rays will usually be normal. An MRI might be ordered to either confirm the diagnosis or to rule out other conditions.
Differential Diagnosis:
- Patellofemoral syndrome (PFJ syndrome)
- Lateral compartment osteoarthritis
- Lateral meniscus tear
- LCL sprain
- Greater trochanteric bursitis
- Hip abductor/adductor strain
- Lumbar pathology (Degenerative disc disease)
Treatment:
Most cases of IT band syndrome can be appropriately managed conservatively, without surgery. The mainstay of treatment is physical therapy to involve active-release therapy (ART) of the affected hip musculature and tensor fascia lata muscle. Modalities include:
- Rest of the affected knee
- Oral and topical anti-inflammatories (NSAIDs ex. Celebrex, Meloxicam, Naproxen)
- Physical therapy
- Steroid injection
Goals of therapy:
- Improve strength and flexibility of the lower extremity musculature, with a primary focus on the IT band, quadriceps, gluteal muscles, and hip abductors.
- Decrease pain, swelling, and atrophy utilizing available modalities
- Increase range of motion and overall lower extremity joint mobility
- Initiate a home exercise program → focus on gluteal and quadricep strengthening routine (daily) in addition to IT band and lower extremity stretching
- Educate patient on pathophysiology of the disorder
- Educate patient on taping techniques
Proprioception exercises can also be used to improve symptoms. Rarely, surgery to release the IT band is indicated. Surgery may include a surgical excision of the iliotibial band or a Z-plasty of the iliotibial band at the knee. Surgery to rarely required to treat this disorder and is only considered in extreme cases that have failed an extended course of conservative management and aggressive physical therapy.
Prevention:
- If you are exercising, increase your activity level gradually.
- Warm up prior to exercise.
- Replace your running shoes every 300 miles.
- Stretch regularly.
- Avoid uneven running terrain.
- Use a foam roll to stretch IT band.
Dr. Dold specializes in the management of all knee and hip conditions including IT band syndrome. To schedule a new patient consultation, please fill out a form and a member of our team will reach out to you within 24 hours to confirm your appointment.
To view Dr. Dold’s Video on the importance of physical therapy click here:
Related Articles:
- Iliotibial band syndrome: evaluation and management.
- Iliotibial Band Syndrome in Runners: Biomechanical Implications and Exercise Interventions.
- Iliotibial Band Friction Syndrome.
- Iliotibial band syndrome rehabilitation in female runners: a pilot randomized study.
- Iliotibial band syndrome.
- A Review of Treatments for Iliotibial Band Syndrome in the Athletic Population.
- Biomechanical risk factors associated with iliotibial band syndrome in runners: a systematic review.
- Iliotibial band syndrome: a common source of knee pain.
- Conservative treatment of iliotibial band syndrome in runners: Are we targeting the right goals?
- Operative Versus Nonoperative Management of Distal Iliotibial Band Syndrome-Where Do We Stand? A Systematic Review.
- Radial extracorporeal shockwave therapy compared with manual therapy in runners with iliotibial band syndrome.
- Hip abductor strength and lower extremity running related injury in distance runners: A systematic review.
- The Iliotibial Band: A Complex Structure with Versatile Functions.
- Iliotibial Band Pathology: Synthesizing the Available Evidence for Clinical Progress.
- The functional anatomy of the iliotibial band during flexion and extension of the knee: implications for understanding iliotibial band syndrome.
- Iliotibial band syndrome in non-athletes.
- Musculoskeletal Injuries in Ultra-Endurance Running: A Scoping Review.
- Differences in Knee and Hip Adduction and Hip Muscle Activation in Runners With and Without Iliotibial Band Syndrome.
- Greater trochanteric pain syndrome: a review of anatomy, diagnosis and treatment.
- Relationship between iliotibial band syndrome and hip neuromechanics in women runners.


